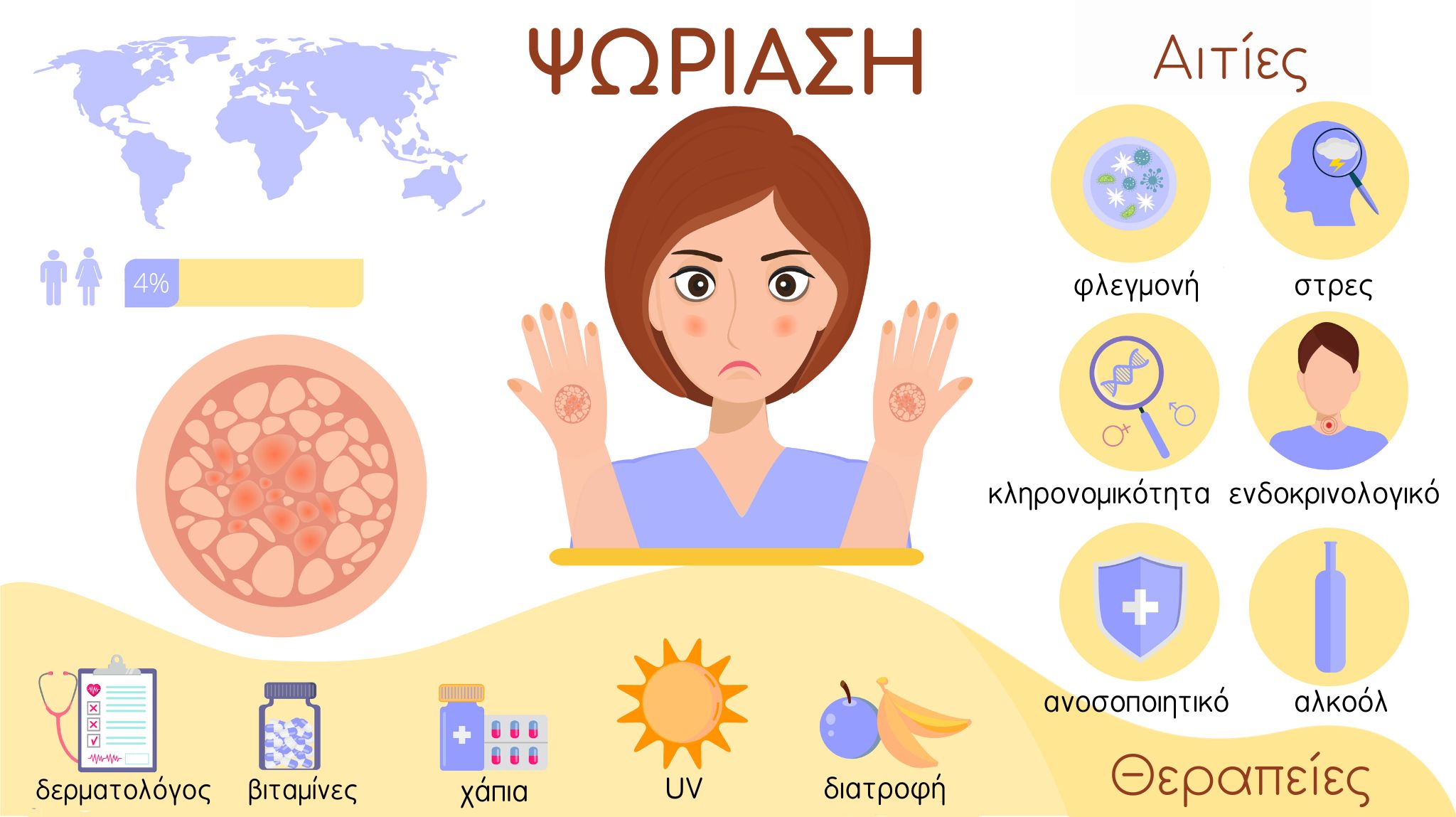
What is psoriasis?
Psoriasis is a chronic, non-contagious disease that appears on the skin, joints, and nails. It is an autoimmune disease, meaning it is caused by an overstimulation of the immune system.
The exact cause of psoriasis is not known, but it is linked to heredity. Of course, there are triggering factors, such as skin injuries, infections and viruses, endocrine factors or taking certain medications, alcohol abuse and even stress.
Symptoms
Psoriasis causes excessive proliferation of skin cells in the upper layer of the skin, resulting in psoriatic plaques - red patches covered with silvery or white scales, i.e. hard to the touch areas with flakes or scales. It appears anywhere on the body but most often in areas such as the elbows, knees, head, and even the palms and soles. The skin is hard and cracked and often itches. Sometimes the patient may develop psoriatic arthritis, which causes pain, swelling and stiffness of the joints. It can also affect the nails.
Living with the disease
As with other chronic autoimmune diseases, psoriasis can affect emotional health, interpersonal relationships, and the way one handles stress. For some people, living with psoriasis can be a challenge, especially in the summer, when we dress lightly or in swimsuits. Because psoriasis is wrongly stigmatized, it is associated with scabies in the minds of many and there is a fear of contagion. As a result, psoriasis patients often experience feelings of anxiety, shame, shyness at the beach, depression, isolation, or fear.
However, there are various ways to manage the disease so that the patient suffering from psoriasis has a quality life and the support they need. It is important to establish the perception in society with proper information that this is not a contagious disease. Many patients consult a psychologist if they feel they need more help with the psychological part of managing the disease.
It is particularly beneficial for psoriasis sufferers to find the right communities and talk to fellow sufferers, because in this way different stories are heard in the light of the common experience of the disease and understanding is broadened. The psychological support that one receives by participating in patient groups offers hope and solidarity. There are patient networks that offer information and support, such as the Panhellenic Association of Patients with Psoriasis and Psoriatic Arthritis, “Epidermia”.
Types of psoriasis and treatment
There are different types of psoriasis, and it is possible for someone to suffer from more than one type at the same time - as well as more than one type during their lifetime.
Monitoring the course of the disease by an experienced psoriasis dermatologist is key to finding the right treatment to keep psoriasis symptoms under control. It is important to make regular appointments for re-evaluation of the treatment you are following to discuss with your doctor how the specific treatment is working and how the body is reacting to it.
As this is a chronic disease, it is important that the patient has - in addition to an excellent Dermatologist - patience, valid information, and the support of family and friends, which can be invaluable.







No comment yet, add your voice below!